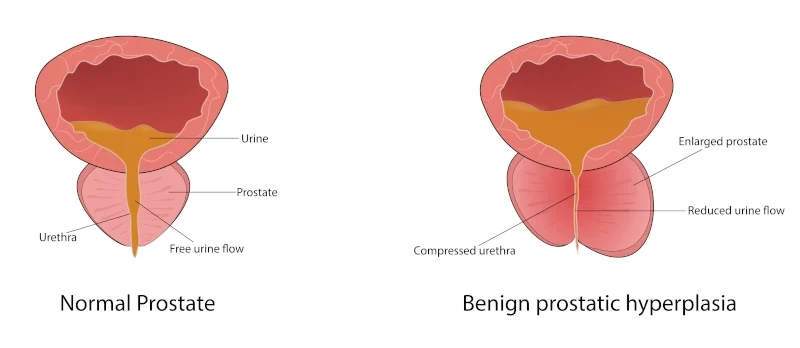
Benign Prostatic Hyperplasia (BPH)
An enlarged prostate (Benign Prostatic Hyperplasia or BPH), is a very common condition affecting nearly all men as part of the male ageing process.
Overview of Benign Prostatic Hyperplasia
Benign prostatic hyperplasia or BPH, is when the prostate gland grows larger than normal. As it gets bigger it compresses the urethra causing lower urinary tract problems such as difficulty emptying the bladder or a weak urine stream.
It is a non-cancerous (benign) condition which is more common in older men, while symptoms can start from 50 years old and is generally caused by age-related cell growth.
While having an enlarged prostate doesn’t increase the risk of prostate cancer, the symptoms of BPH can mimic those of prostate cancer. For this reason, if you have any symptoms associated with an enlarged prostate we urge you to seek medical advice.
The Urology Partnership provides fast access to specialist care, using advanced diagnostics and technology to effectively treat BPH.
Please call us on 0118 920 7040 to arrange an appointment.
What Is The Prostate?
The prostate is a small, walnut-sized gland located just below the bladder and in front of the rectum. Divided into two lobes, it encircles the upper portion of the urethra – the tube within the penis that allows passage of urine and semen.

The prostate’s primary role is to produce a milky fluid that nourishes sperm and aids in its transportation. As part of this process, the gland secretes a protein known as prostate-specific antigen (PSA), which helps liquefy the semen.
Because PSA is produced specifically by prostate cells, a blood test can be used as a marker for prostate health. A rise in PSA levels typically indicates a localised issue within the prostate itself, such as:
- Inflammation or infection: Conditions like prostatitis.
- Benign growth: Non-cancerous enlargement (BPH).
- Malignancy: The presence of prostate cancer.
By measuring these levels, our consultants can determine if further investigation – such as an MRI or biopsy – is required to ensure your long-term health.
Find out more about raised PSA.
What Happens When The Prostate Enlarges?
The prostate is normally 20-30ccs when a man is in his 20s or 30s. It is naturally the shape of a ring-doughnut with the bladder emptying and the urine passing through the middle of the doughnut ring.
As the prostate enlarges, the hole through the middle of the prostate becomes smaller, obstructing the flow of urine and the natural emptying of the bladder.
Enlarged Prostate Symptoms
Early signs of an enlarged prostate are most commonly associated with lower urinary tract symptoms (LUTS) which include:
- Voiding or emptying: A slow, stop-and-starting /intermittent stream, or leaking urine after finishing.
- Straining or hesitancy: Difficulty or delay in starting to empty the bladder.
- Incomplete emptying: A feeling like your bladder isn’t fully empty after urinating.
- Urinary frequency: The bladder may experience difficulty storing urine, resulting in the need for the bladder to empty frequently during the day or night (nocturia).
- Urinary urgency: The need for the bladder to empty in an urgent manner, giving little time to get to the toilet or postpone urination.
In more serious cases of benign prostatic hyperplasia, men may also notice:
Blood in Urine (Haematuria)
As the growing gland puts pressure on the urethra and bladder, it can cause blood vessels to become stretched and potentially bleed. This can cause blood to appear in the urine.
Urinary Tract Infections (UTIs)
UTIs frequently stem from BPH due to two primary factors. First, when the bladder fails to empty completely, the remaining “stagnant” urine becomes a breeding ground for bacteria. Second, the intense pressure required to push urine past an enlarged prostate can actually force fluid back into the prostatic ducts. This backward flow can trigger inflammation and secondary infections, such as prostatitis.
Causes Of An Enlarged Prostate Gland
While it’s not fully understood what causes the prostate to increase in size it is believed key risk factors include:
- Aging: A natural growth phase that continues throughout life.
- Family history: Having a father or brother with an enlarged prostate increases your risk.
- Hormonal changes: As men age, testosterone levels decline while oestrogen levels remain stable or increase, altering the ratio to favour oestrogen-driven growth.
- Diabetes and heart disease: Studies show connections between BPH and diabetes, high blood pressure and metabolic syndrome.
- Lifestyle: Obesity, lack of exercise and poor diet (high in alcohol, caffeine and red meat).
In this short video, Urology Consultant Mr Chris Blick provides an overview of the causes and common symptoms of an enlarged prostate gland.
Our Diagnostic Approach To BPH
Before beginning any treatment, our specialists at The Urology Partnership conduct a thorough evaluation to differentiate benign prostatic hyperplasia from other conditions, such as prostatitis or prostate cancer. This ensures your care plan is precise and effective.
1. Initial Clinical Consultation
- Symptom mapping: We begin with a detailed discussion of your urinary habits. We look specifically for signs of lower urinary tract symptoms (LUTS), including urgency and nocturia.
- IPSS assessment: To objectively measure how much these symptoms affect your quality of life, we use the International Prostate Symptom Score (IPSS). This provides a baseline to track your progress after treatment.
- Physical examination (DRE): A digital rectal exam (DRE) allows your consultant to manually assess the size and texture of the prostate. This quick, routine check is vital for identifying any physical irregularities or tenderness.
2. Advanced Diagnostic Testing
To provide a complete picture of your urological health, we may perform the following:
- PSA blood screening: We measure prostate-specific antigen levels with a simple blood test. While elevated PSA can occur with BPH, it also serves as a key indicator for potential further investigation.
- Urinalysis & flow studies: By analysing a urine sample and performing Urodynamic testing (such as uroflowmetry), we can rule out infections and measure the physical strength of your urinary stream.
- PVR (post-void residual) ultrasound: This non-invasive scan determines if your bladder is emptying effectively or if stagnant urine is remaining behind – a common cause of recurring UTIs.
3. Specialist Imaging and Direct Visualisation
- Multiparametric MRI: If there is any clinical uncertainty, we will organise a high-resolution MRI scan to visualise the prostate tissue in detail.
- Flexible cystoscopy: In some cases, a consultant may use a thin, fiber-optic camera to inspect the internal lining of the bladder and urethra. This can help rule out urethral stricture and visualise your prostatic anatomy to help tailor treatments.
Treating An Enlarged Prostate
At the Urology Partnership choosing the right BPH treatment is a highly individualised process. Using your diagnostic data, our consultants will recommend the most effective treatment for your unique case.
Key considerations when making the choice include symptom severity, preservation of sexual health, prostate size and recovery times.
Management of Mild BPH Symptoms
Where symptoms are mild and not causing many problems, lifestyle changes are usually recommended first. This may involve losing weight, eating healthily, exercising more, and reducing alcohol and caffeine intake. You may also be given a programme of pelvic floor exercises to strengthen the muscles that help control the bladder.
Minimally Invasive Enlarged Prostate Procedures
If lifestyle changes are insufficient, we offer a range of advanced procedures focused on providing relief from the symptoms of BPH, faster recovery and better preservation of sexual and urinary function:
Rezum (Water Vapor Therapy): Uses steam (water vapour) to destroy obstructive prostate tissue, shrinking the gland with minimal disruption. The procedure takes approximately 20 minutes and is usually performed as day surgery.
UroLift System: A revolutionary approach to treating an enlarged prostate that uses tiny implants to hold the enlarged prostate tissue out of the way so it no longer blocks the urethra. There is no cutting, heating or removal of prostate tissue, preserving sexual function.
Prostate Artery Embolization (PAE): A day-case image guided non-surgical procedure which uses tiny particles to block off blood flow in the arteries that feed the prostate gland, causing it to shrink. Studies show long-lasting symptom improvement and fewer sexual side effects than surgery.
Advanced Surgical Solutions For BPH
For significantly enlarged prostates or complex cases, we utilise “gold standard” surgical techniques:
Aquablation Therapy: An innovative surgical procedure that uses a robotic system and a heat-free, high-velocity waterjet, guided by ultrasound, to precisely remove excess prostate tissue and reduce risks of sexual side effects.
Holmium Laser Enucleation of the Prostate (HoLEP): An advanced treatment recommended for men with very large prostates (over 80-100cc). The procedure uses a high-energy Holmium Laser to separate the central part of the prostate from the surrounding fibrous covering (capsule). Benefits include high long-term effectiveness, reduced bleeding and faster recovery times.
Transurethral Resection of the Prostate (TURP): Considered one of the best options for the surgical treatment of BPH, TURP is a minimally invasive procedure which involves removing the inner portion of the prostate gland to relieve obstruction to the flow of urine through the prostate.
BPH Treatment Comparison Matrix
The table below provides a quick summary of the key differences between our six primary treatment pathways.
| Treatment | Tech Type | Best For... | Typical Recovery | Sexual Function Risk |
|---|---|---|---|---|
| Rezum | Water Vapor (Steam) | Moderate enlargement (30-80cc) | 3–5 days | Minimal: High preservation of all functions. |
| UroLift | Mechanical Implants | Lateral lobe obstruction | 1–2 days | Lowest: No tissue removal; preserves all functions. |
| Aquablation | Robotic Waterjet | All sizes; complex shapes | 2–4 days | Low: Robotic precision helps spare ejaculatory ducts and reduces chance of losing ejaculation |
| PAE | Embolisation | High-risk surgical patients | 1–2 days | Very Low: Non-surgical approach via blood vessels. |
| HoLEP | Holmium Laser | Large to Very Large (100cc+) | 1–2 days | Moderate: High risk of retrograde ejaculation |
| TURP | Electrical Resection | Moderate-sized glands | 1–2 weeks | Moderate: High risk of retrograde ejaculation (dry orgasm). |
Next Steps: Find Relief From BPH Symptoms
When it comes to prostate health, the right expertise can make a significant difference in your long-term quality of life. At The Urology Partnership, we combine world-class surgical skill with a compassionate, tailored approach to men’s health.
Contact The Urology Partnership today to arrange a private consultation with one of our specialists.
Call: 0118 920 7040
Email: info@theforburyclinic.co.uk
Location: The Forbury Clinic, 11 Kendrick Road, Reading, Berkshire.
FAQs
While an enlarged prostate is the usual culprit behind urinary changes in men, it isn’t the only possibility. Prostate cancer can sometimes present with similar signs like a weak flow or needing to frequently urinate. However, other causes such as urinary infection or overactive bladder can also cause symptoms.
As it is difficult to distinguish between benign prostate growth and more serious conditions based on symptoms alone, any shift in your regular bathroom habits warrants a conversation with a medical professional
While an enlarged prostate isn’t a direct physical cause of erectile dysfunction, the two often occur together as men age.
The secondary effects of BPH – such as sleep deprivation from frequent nighttime bathroom trips and the resulting stress – can significantly dampen sexual desire and performance.
Because modern treatments like Aquablation Therapy or Prostate Artery Embolisation (PAE) can address BPH symptoms, a consultation with a specialist is the recommended first step.
In younger men, the focus is often on high-speed recovery and the preservation of sexual function. Treatments most suitable for this health goal include:
Rezum (Water Vapor Therapy):
- Best for: Men seeking a quick, day-case procedure with minimal downtime.
- Suitability: Prostates between 30cc and 80cc, including those with a middle (median) lobe.
- Key benefit: Extremely low risk of sexual side effects; preserves natural ejaculation.
UroLift System:
- Best for: Men who want to avoid any cutting, heating or removal of tissue.
- Suitability: Ideally suited for lateral lobe enlargement under 80cc.
- Key benefit: Immediate results with virtually zero risk of new, permanent sexual dysfunction.
Aquablation Therapy:
- Best for: Men with larger prostates who still prioritise sexual health.
- Suitability: Effective for a wide range of sizes, including large glands up to 150cc.
- Key benefit: Robotic precision ensures high-velocity waterjets remove tissue accurately, sparing the ejaculatory ducts. Loss of ejaculation could still occur however in about 10-15%, which is lower than the 70% seen in TURP.
For larger glands, more robust tissue removal or reduction is required to ensure long-lasting relief. Suitable treatments include:
Aquablation Therapy:
- Best for: Men with larger or unusually shaped prostates who still prioritise sexual health.
- Suitability: Effective for a wide range of sizes, including large glands up to 150cc.
- Key benefit: Robotic precision ensures high-velocity waterjets remove tissue accurately, sparing the ejaculatory ducts. Loss of ejaculation could still occur however in about 10-15%, which is lower than the 70% seen in TURP.
HoLEP (Holmium Laser Enucleation):
- Best for: Very large prostates or men in complete urinary retention.
- Suitability: The “size-independent” solution; effective for any prostate size.
- Key benefit: Removes the most tissue possible with the lowest risk of regrowth. The most effective operation at unblocking prostate tissue and giving excellent flow.
TURP (Transurethral Resection):
- Best for: A reliable, time-tested approach for moderate-sized glands.
- Suitability: Historically the “gold standard” for men who are not candidates for newer laser therapies. Usually performed on glands up to 80cc.
- Key benefit: Decades of clinical data and high success rates for clearing the urinary path.
PAE (Prostate Artery Embolisation):
- Best for: Patients who prefer a non-surgical approach or those who may not be suitable for general anesthesia.
- Suitability: Often used for very large prostates or for patients with complex medical backgrounds.
- Key benefit: An interventional radiology procedure performed via a small catheter in the groin/wrist; no “surgery” in the traditional sense.
Next Steps
Get fast access to leading specialists for the swift diagnosis and treatment of urological conditions in a private clinic environment.
If you would like more information or wish to arrange a consultation with one of our specialist consultant urological surgeons then please either Call 0118 920 7040 or complete the form below.
Insured patients
Contact your GP and ask for a referral to the Urology Partnership.
All consultations, investigations and treatments are covered by major insurance companies (depending on policy).
Funding your own treatment
Self-funding initial consultation fee is £250. Follow up fees are £175.
Consultation charges are exclusive of any tests and other investigations that the consultant may wish to carry out.